-
Get Control of Your Acne
posted: Apr. 26, 2022.
Patients seek out Advanced Dermatology and Mohs Surgery to treat their acne in Batavia, IL. Acne is extremely common and can happen at any age, so you're not alone if Read more -
Ways a Dermatologist Can Help You Get Rid of Warts
posted: Apr. 25, 2022.
Advanced Dermatology and Mohs Surgery is here for all your skincare needs. Dr. Sharon Horton helps patients struggling with warts in Batavia, IL. Keep reading about warts and come see Read more -
The Benefits Of Seeing A Dermatologist
posted: Apr. 20, 2022.

-
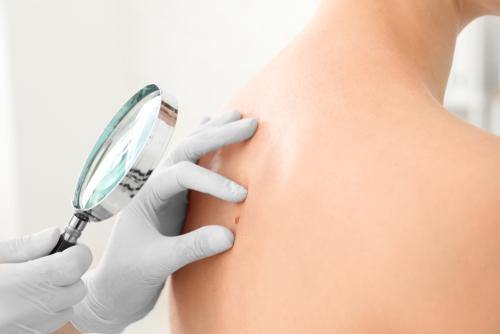
Skin Cancer Prevention And Early Detection
posted: Apr. 07, 2022.
-
Treating Your Birthmarks
posted: Mar. 28, 2022.

-
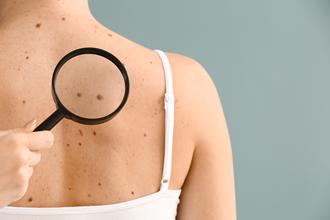
Do I Have an Irregular Mole?
posted: Mar. 09, 2022.
-
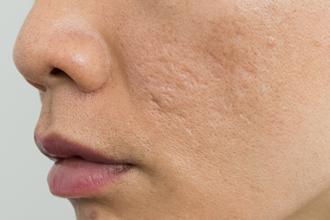
Finding Treatment for Facial Scarring
posted: Feb. 24, 2022.
-
Screening for Early Skin Cancer: Know your Risks
posted: Feb. 18, 2022.
Could you benefit from a skin cancer screening? When was the last time you had a skin cancer screening? Perhaps the better question might even be, “Have you ever had a Read more -
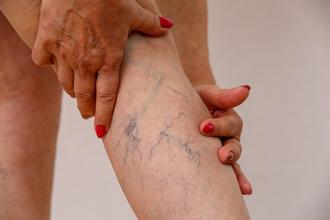
What Are Spider Veins?
posted: Feb. 03, 2022.
-
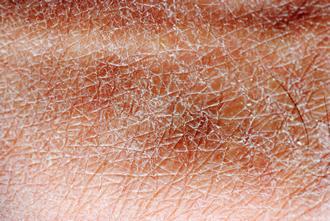
How To Treat Dry Skin
posted: Jan. 21, 2022.
-
How To Prevent Psoriasis From Spreading?
posted: Jan. 18, 2022.
Preventing the spread of itchy, red, scaly patches can be a challenge when you have psoriasis. Fortunately, your dermatologist in Batavia, IL, Dr. Sharon Horton, offers treatments that can slow Read more -
Treating Your Vitiligo
posted: Jan. 07, 2022.

-
Mohs Surgery FAQs
posted: Jan. 07, 2022.
Have questions about Mohs surgery? If you or someone you love has just been diagnosed with melanoma or non-melanoma skin cancer, our Batavia, IL, dermatologist Dr. Sharon Horton may have recommended Read more -
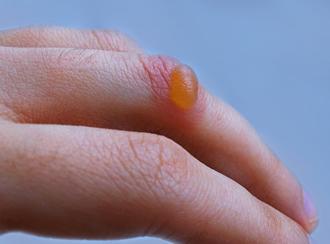
How To Treat Your Blisters
posted: Dec. 21, 2021.
-
Treating Persistent Acne
posted: Dec. 20, 2021.
Is it time to turn to our Batavia, IL, dermatologist to treat your acne? Acne is one of the most common skin problems that our Batavia, IL, dermatologist Dr. Sharon Horton Read more -
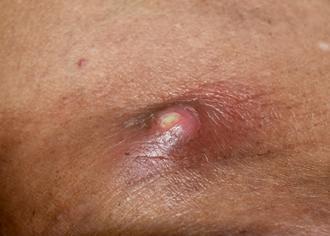
What Is a Carbuncle?
posted: Dec. 09, 2021.
Blog

Office Hours
Monday:
8:30 am-5:00 pm
Tuesday:
8:30 am-5:00 pm
Wednesday:
8:30 am-5:00 pm
Thursday:
8:30 am-5:00 pm
Friday:
9:00 am-3:00 pm
Saturday:
Closed
Sunday:
Closed
